Understanding Medicare Advantage Plan & AI’s Role in Compliance
TL;DR, Medicare Advantage Plan or MA market is fast-changing and highly competitive. According to the Chartis Report of 2023, Special Needs Plans (SNPs) have driven much of the market’s growth this year which reflects changes in beneficiary needs and insurer strategies. However, with time SNPs are expected to expand and this makes it essential for healthcare providers to participate in Medicare Advantage (Part C). In addition, they must adapt to evolving policies. Because Plan C requires providers to contract with private insurers and this means following different reimbursement rates, coverage policies, and compliance rules set by each insurer. All these variations put healthcare providers at challenge in understanding policies, manage claims and handle denied claims. To get the maximum benefits, providers must know and follow guidelines of the medicare advantage plan. This guide explores key changes, challenges, and how AI in healthcare like Policy Copilot can help providers navigate these complexities in a quick way.
Understanding Medicare Advantage Plan
Medicare is a federal health insurance program in the USA. However, Medicare Advantage (MA) plans, or Medicare Part C, are private alternatives to traditional Medicare, funded by the federal government. It is primarily for people aged 65 and older but it is not limited. It is also for some younger individuals with disabilities.
According to statista report of 2023, over 50% of Medicare beneficiaries were enrolled in MA plans, with UnitedHealthcare leading at 8.9 million members. However, the latest report shows that the MA spending share was projected to reach 62 percent of Medicare in 2025.
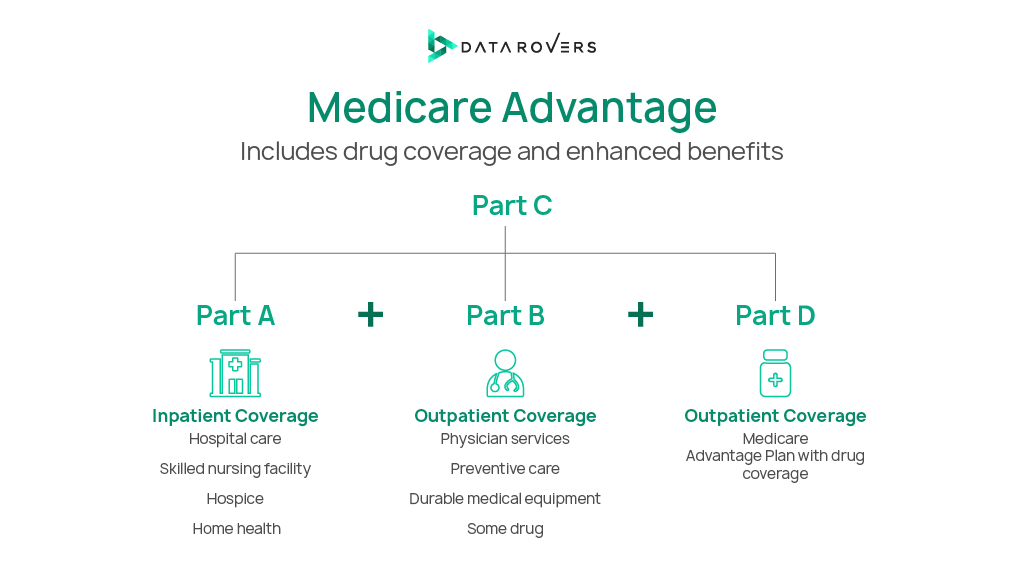
Types of Medicare Advantage Plan
Medicare Advantage has different plans and its types. Each type has a unique structure and coverage rules. Healthcare providers must know updates on policy changes as contractors with insurers set reimbursement rates and participation terms. Here are some of the plan types:
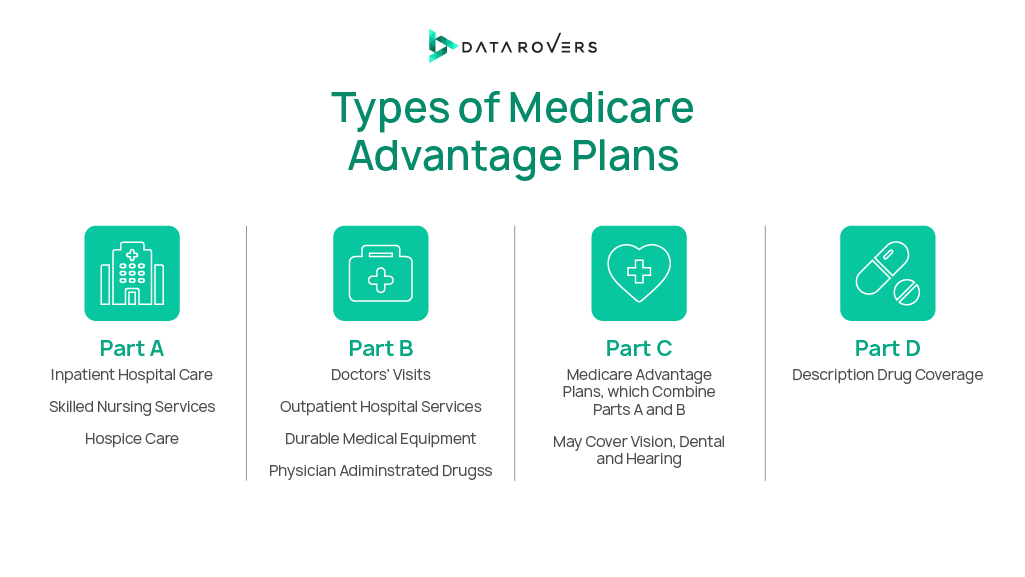
- Health Maintenance Organization (HMO) plans require members to use in-network providers and obtain referrals for specialist care.
- On the other hand, Preferred Provider Organization (PPO) plans offer more flexibility but at higher costs for out-of-network services.
- Private Fee-for-Service (PFFS) plans allow enrollees to visit any provider that accepts the plan’s terms.
- Moreover, Special Needs Plans (SNPs) cater to individuals with specific chronic conditions or institutional care needs.
- Lastly, Medical Savings Account (MSA) plans combine high-deductible health insurance with a savings account to cover medical expenses.
In simple terms, we can call them plan a, plan b, plan c and plan d. Let’s categorize them in a table for a streamlined view:
| Medicare Part A
(Hospital Insurance) |
Medicare Part B
(Medical Insurance) |
Medicare Part C (Medicare Advantage) |
Medicare Part D
(Drug Coverage) |
|---|---|---|---|
| Covers inpatient hospital stays, skilled nursing facility care, hospice care, and home health care services. | Covers outpatient care, doctor visits, preventive services, and home health care. | An alternative to Original Medicare (Parts A and B) offered by private insurance companies approved by Medicare. | Provides prescription drug coverage to help beneficiaries pay for self-administered prescription medications. |
| Beneficiaries don’t need to pay a premium for Part A if they or their spouse have paid Medicare taxes for a certain period. | Beneficiaries pay a monthly premium for Part B coverage.
|
These plans often include additional benefits such as dental, vision, and hearing coverage, and may incorporate prescription drug coverage (Part D).
|
This coverage is offered through private insurance companies.
|
Medicare Advantage Plans Challenges For Healthcare Providers
Medicare Advantage plans pose different challenges for providers, but one of the biggest hurdles is the complexity of payer policies. First, it changes frequently which makes compliance difficult. Second, it intensifies administrative burdens that increase paperwork and prior authorization requirements consuming valuable time. Third, it affects revenue cycle inefficiencies with delayed payments and higher claim denial rates. Lastly, MA plans often reimburse providers at lower rates than traditional Medicare. All of these create financial strain for healthcare organizations.
Navigate Changes of Medicare Advantage Plans Efficiently – But How?
The only answer is automation and digital transformation in healthcare processes. DataRovers designed a Healthcare Policy Software called Policy Copilot or LUNA. It is an automated Medical Policy Management that helps in retrieving payor guidelines in minutes.
Integrating LUNA AI Policy Copilot can help healthcare providers by offering an extensive policy database. This app ensures easy access to updated payer policies and Medicare guidelines. Moreover, it provides;
- Instant notifications to providers as alerts about crucial policy changes that impact claims and reimbursement processes.
- The system also includes a chat history feature which allows providers to reference past queries and documentation.
Improve Efficiency With LUNA Policy Copilot
Integrate Policy Copilot today and improve efficiency through automation and AI-driven technology. It will give you updated policy information, generative AI, and real-time analytics. If you are a healthcare provider, RCM professional or a C-level in healthcare organization, it will help you streamline compliance efforts, reduce administrative burdens, and optimize reimbursement processes.

As you know, administrative costs and regulatory complexity is increasing, investing in digital tools like Policy Copilot will sustain operational efficiency and ultimately enhance patient care. In this case, Medical necessity insights, powered by AI and trained on CMS and FDA guidelines are proven to be helpful for providers in determining which procedures are covered under specific conditions. Moreover, with HIPAA-compliant security measures, Policy Copilot ensures data privacy while streamlining healthcare policy management.
Conclusion
As Medicare Advantage Plans especially, (Part C) becomes essential for healthcare providers to adapt. Similarly, staying informed about constantly updating policies from payers and insurers is important. However, staying updated and reading out policy updates everyday presents a significant challenge. Moreover, frequent changes in reimbursement rates, coverage policies, and compliance requirements add to administrative burdens and increase the risk of claim denials. So what’s the solution? AI-driven solutions like LUNA Policy Copilot can automate policy tracking, provide real-time updates, and simplify compliance. This support helps providers reduce administrative burdens, ensure compliance, and minimize claim denials, ultimately leading to more efficient operations and improved patient care.
Automate Policy Management for Healthcare Providers and Get Smoother Operations & Improved Financial Outcomes! Get a Demo Today
FAQs
1. What challenges Medicare Advantage Plans pose for healthcare providers?
Medicare Advantage Plans are constantly changing in policies, reimbursement rates, and compliance rules. It makes it difficult for providers to stay informed and manage claims efficiently.
2. How can AI improve Medicare Advantage Plan management?
Integrating tools like LUNA Policy Copilot that are AI-powered can automate policy management and tracking. It provides real-time CMS, Medicare and other Private Payers updates, and helps simplify compliance, reducing administrative burdens and claim denials.
3. What makes Policy Copilot essential for Medicare Advantage Plans?
Policy Copilot by DataRovers has a significant importance in healthcare as it helps providers navigate Medicare Advantage Plans by offering instant payer policy updates in one click. Ask Questions and get instant replies with reference documents.




